Shortage of Blood: Flourishing Illegal Blood Supply Market in India
- carolina9384
- Dec 22, 2021
- 22 min read

If you are interested to apply to GGI Impact Fellowship, you can access our application link here.
Abstract
India's blood industry is characterised by several problems like shortage of blood supply, ambiguous laws, distribution inefficiencies and blood wastage. This has driven the creation of an illegal blood market. After analysing the blood infrastructure, we propose recommendations to increase the supply, improve the regulatory framework, develop an equitable distribution network and transform the management of blood in India, using technologies such as Big Data and blockchain.
1. Introduction
The objective of this paper is to analyse the blood market in India & provide recommendations in improving the overall efficiency & effectiveness of the same. To achieve this, we start with a definition of a few important terminologies such as population need, clinical demand, supply & utilisation & its current status in India.
We then do a comparative analysis with our international counterparts on the status of blood availability & the rate of donation. This understanding of the current scenario sets the stage for further analysis of the problems associated with the blood market by delving deeper into the blood donor issues, distribution inefficiencies & bottlenecks, wastage of blood, etc.
Thereafter, we delve deeper into analysing the supply chain of the blood market by mapping different stakeholders involved in the entire process & thereby identifying gaps at every stage of blood delivery. Detailed study of the current legal architecture that monitors & regulates the blood market constitutes the next important segment in the analysis.
Through our problem analysis & understanding of the current legal structure, we then establish the causes & repercussions of the illegal blood market in India. This understanding becomes foundational for a series of short-term and long-term recommendations that would help in enhancing the availability and ensuring equitable distribution of blood in the Indian ecosystem.
2. Only 76% of the clinical demand for blood is met!
Blood Transfusion Service (BTS) is a critical component of any health care delivery system. Policy makers at different levels, civil society & providers of blood for transfusion need to know how much blood is required for their population, where and when it is needed so that blood is neither under- nor over- supplied. This calls out for developing a conceptual framework that can be developed by defining a few important terminologies, viz. population need, clinical demand, supply & utilisation & looking at what their current status in India is. This in turn would be helpful in quantifying need-demand, demand-supply & supply-utilisation gaps & thus setting the stage for finding potential causes of the same.
Population need is defined as the total number of blood units (whole blood or components) that are required to transfuse all individuals who require blood transfusion in a defined population over a defined time period. This requirement depends on the burden of diseases & clinical interventions that require a blood transfusion if there is universal access to health care services.
Current clinical demand for blood is defined as the total number of blood units (whole blood or components) that is requested/demanded at a defined number of health facilities to meet all blood transfusion for emergencies and elective procedures over a defined time period. It depends on the capacity of the healthcare system & is rarely achieved in low-resource settings, resulting in gaps between the need & demand for blood. This could be due to several factors such as lack of awareness, lack of clinicians’ knowledge/skills in suggesting if the condition requires BTS & apprehension, hesitancy & lack of trust from the general populace in health institutions (overall health-seeking behaviour of the population). All these factors pose a huge challenge in availing BTS.
Current supply of blood is the total number of units of whole blood & components supplied to healthcare facilities, against all requests/demand for blood transfusion over a defined time period, usually taken as one year. The supply of blood is generally from licensed blood banks or blood storage centres across the country. There exists a gap between clinical demand & supply due to the lack of healthcare access & infrastructure, low volume of voluntary blood donation, irrational demand, poor supply chain management system etc.
Current utilisation of blood is the total number of whole blood units & components utilised by a defined number of healthcare facilities over a defined period, usually one year. There may be a gap between supply & utilisation due to wastages, expiry, non-utilization in the health facilities.

Figure 1
The huge need-demand gap as shown in figure 1, requires an intervention that is multi-sectoral in nature & hence filling up this gap should be our long-term goal. The analysis & study of this gap falls outside the purview of this paper since the scope is too broad-based to cover. In this paper, we focus primarily on the reasons behind the demand-supply gaps & supply-utilisation gaps that exist in the blood market of India & recommendations to bridge that gap. The demand-supply gap in India is quite high with only 76% of the demand being met by supply as represented in figure 1.
From the global perspective, the blood shortage issue is not exclusive to India. In this regard, it is imperative to compare the status of blood availability & donation rate in different countries to understand the level of disparity in blood supply against population on a global level. Globally, less than 45% of the donated blood annually is collected in developing countries which are home to about 80% of the world’s population. This directly shows us the skewed nature of blood as a commodity with the supply being low from developing countries. In addition, WHO’s global status report on blood availability shows that there is a mismatch in donation rate and population of South East Asia Region (SEAR) and in Lower Middle-Income Countries (LMIC) as shown in Figure 2.
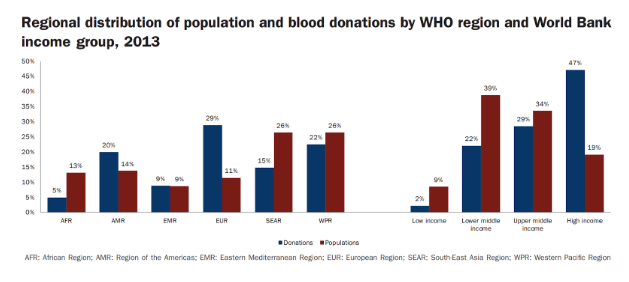
Figure 2

Figure 3
However, the South East Asian Region has seen a major increase in the millions of units of blood collected, an increase of 75% in the Voluntary unpaid donations.This increase is because of India with a large change of 85% from 4.6 to 8.5 million units collected within the same timeline. But these numbers do not tell the entire story. India in 2016 had a donation rate per 1000 population in the range of 5 to 9.9 as shown by Figure 3. The donation rate per 1000 population that India must achieve to meet all the population need & the clinical demand is 20.1 & 11.2, respectively as shown in table 1. The current donation rate per 1000 population is only 8.4 (annual collection in 2017 reported by NACO) as shown in table 1 & this indicates that India still doesn't have enough supply of blood in the country.

Table 1
3. Issues of Insufficient number of donors and poor donor retention lead to loss in supply
3.1. Insufficient donors
Multiple research papers, based on surveys of Indian people across different ages and demographics, reveal that there is a lack of motivation amongst the Indian population to donate blood. This leads to low voluntary blood donations in India among first-time donors. The available blood supply from first-time donors gets further reduced due to donor deferrals.
1. Low voluntary blood donations
The lack of interest among potential first-time blood donors, can be explained by a lack of both intrinsic and extrinsic motivation which are described as follows:
Intrinsic factor: Intrinsic factors of motivation refer to reasons internal to the potential donor, for not wanting to donate blood. Fear was the intrinsic factor dominant among such donors. Potential donors mentioned having fears of being pricked by syringes, as well as fears of contracting HIV/AIDS and other transmissible diseases during the donation process. Certain potential donors also mentioned the consequent weakness after blood donation, as a deterrent.
Extrinsic factors: These refer to external circumstances that influence the motivation of the blood donor to donate blood. These are best explained by a lack of awareness, accessibility, and affordability, about blood donation.
Lack of awareness: There exists considerable misinformation about the blood donation process. The false beliefs are that blood donation is associated with a loss of fertility; it causes permanent weakness and accelerated ageing. The fear of these alleged side-effects of blood donation, leads to lesser willingness to donate blood.
Lack of accessibility: Lack of accessibility to blood donation was underlined by a lack of situational desire to donate blood. Some donors never faced a situation where they were required to donate blood.
Lack of affordability: Donors could not afford to donate blood because of its time-consuming nature. They either do not see the investment of time as worthwhile, or have schedules that are too busy for them to devote time to blood donation.

Figure 4
2. Donor deferral
This analysis is done with respect to the donor profiles. The donor profile refers to the age group range for different donors. The analysis was done by WHO, for a global scale and reflects the major issues in the region.
The following two images talk about the major profile that contributes to the blood donation and the donation rate for a particular age group.

Figure 5: Contribution to donations by donors of different age groups, 2013

Figure 6: Age groups donation rate (per 1000 population), by World Bank economic group, 2013
In total blood units collected in Lower Middle-Income Countries, the maximum contribution is from the age group 25 to 44. But when we look at the age group’s donation rate (per 1000 population) we see that it’s less than 10, meaning we are not able to tap into the donation potential of that age group. Ideally, we would want 100% donations from that age group but that can never be the case, as shown by the donor deferral data.
Donor deferral means postponement or permanent exclusion of a particular donor based on certain criteria which affects the total maximum potential of the donor's pool. The deferral data across the globe has a range from 1% to 37% with the median being 12%. India has a donor deferral of 11.2%. The criteria for donor deferral are donor’s health might be affected by donating (mostly because of low haemoglobin), risk of a transmitting transfusion transmissible infections, a condition where transmissibility by blood is unknown or donors with diseases or a condition not suitable for blood donation and Sensitive physical and social considerations making donors non suitable for blood donation.
3.2. Poor donor retention
Donors who had donated blood at least once, mentioned the following as reasons why they were not motivated to donate blood again:
Bad past donation experience: The donation experience was plagued by impolite behaviour of the staff, long waiting times and inconvenience caused during the process. This reduced the desire of donors to donate blood more in the future.
Poor ambience of the blood donation centre: The donors disliked the ambience of the physical setting where they had to donate blood. Some of them mentioned it as ‘being unhealthy’ while others did not like the ‘unpleasant atmosphere’. Bad infrastructure- physical aspects of the centre are to blame.
Thus, the problem lies not just in getting first-time donations, but also in getting repeat donations. As of 2020, the proportion of repeat donations is 30% at maximum.
4. Distribution is fragmented and inefficient which adds fuel to the fire
The existing blood infrastructure depends on a functional blood bank, near every hospital in the country, which can be accessed and has a large, pre-screened pool of blood available at all hours of the day. India also experiences a significant rural–urban disparity in distribution of blood supply. Even though 68% of the country’s population is rural, most of its blood banks are in urban areas. There are some 80 districts that have no access to any blood bank whatsoever. Consequently, there is a lack of supply of blood products and its components like plasma in the existing blood banks.
The system fails to provide timely access to safe blood for patients in rural India:
The system requires a family member of a patient in urgent need of blood transfusion to travel to the nearest blood bank, which is often hours away.
If the blood bank has an insufficient supply of blood, the family members must furnish a willing, healthy replacement donor as per the government’s regulations. Quite often the patients are unable to procure a replacement donor and are thus reliant on non- voluntary or commercial donors increasing their risk of Transfusion Transmitted Infections (TTIs). They must then navigate the process of donating blood and obtaining proof of donation before travelling back to the hospital, blood in hand. It results in extensive delays for patients urgently in need of blood products.
The high cost of travel and blood transfusion makes the system unaffordable for many patients.
Due to the lack of voluntary donations, the blood banks themselves rely on illegal commercial donors, thereby Increasing the overall risk of TTI within India’s blood bank supply pool.
4.1. Blood Storage Centres are not operational in rural areas
Facilities where blood is not collected but is acquired from central blood banks and stored—were introduced in 2001 to increase access in such geographically remote areas. In India, only Regional Blood Transfusion Centres (RBTCs) are allowed to open storage centres, and only a small number of blood banks are accredited as RBTCs. Some rural surgeons also attest that in many public hospitals, blood storage centres exist only in name. These centres are rarely operational due to factors like the replacement donors and preferential deferral of nearly expired or unwanted blood group units to the storage centre.
In addition to the above challenges, blood banks require constant and reliable power supply to operate the blood storage refrigerator and other necessary appliances. The lack of these facilities in rural areas leads to wastage of blood which is even more significant when the blood needs to be transported from one of the central banks to storage centres at certain temperatures over long distances.
The rural and remote areas have to bear the brunt of this inefficacy. Given their lack of resources and available knowledge to such systems, rural areas become an easy breeding ground for organised commercialised blood donors.
5. Wastage of blood contributing to shortage in supply
Countries in Lower Middle-Income Countries face the worst among other income divisions in terms of discard of blood, with a median of 10.9% as discard rate. Such countries have the major reasons being reactivity for markers of transfusion-transmissible infection (TTIs) and expiry of use (specifically for platelets).

Figure 7: Distribution of discards of blood donations by reason, 2013
India wastes approximately 6.5 lakh units of blood and blood components each year. This is roughly in the estimated range of 4% to 7% range of discard of blood as per the research.
6. Patients can receive blood in either legal or illegal ways
Presented below is the stakeholder mapping of the Indian blood market.

Figure 8
Stakeholder mapping helps identify every possible determinant of demand and supply of blood in the Indian blood market. This thereby builds a storyline around the journey of a blood bag from creation to discard. It also sheds light on the difference between the intended functioning of the blood market and the actual functioning.
7. Ambiguous legal and regulatory infrastructure
Blood transfusion services in India are regulated by the Drugs and Cosmetics Act (DCA), 1940 which specifies accommodation, manpower, equipment, supplies and reagents, good manufacturing practises, & process control to be followed in Indian blood transfusion services. Regulatory affairs in the Indian blood banking system are controlled by the Union and state Drug Control authority under the Drug Controller General of India (DCGI). The act of selling or donating blood in exchange for money is illegal under the National Blood Transfusion Services Act 2007. Blood banks are also required to obtain a dual licence by both federal and state regulatory bodies as per the Govt. of India’s mandate in 1993, with a renewal required every 5 years. This is a significant barrier to entry for new blood banks and blood storage centres.
The DCA also licensed blood as a drug which established minimum standards of space, people, and equipment and support for blood safety from the National Aids Control Organisation (NACO). While the pharmaceuticals controller is the regulatory organisation often overburdened with medications and clinical trials, NACO/National Blood Transfusion Council (NBTC) have the technical capacity to govern and supervise the blood transfusion services. However, their function is that of an adviser. As a result, while the pharmaceuticals controller efficiently monitors the legal requirements of infrastructure, equipment, spacing, and staff, the medical and quality components of transfusion medicine are disregarded.
In addition to this, even though all blood banks are licensed, the Drugs and Cosmetics Act has not been updated to include the latest procedures, putting reliability at risk.
The cumbersome Government Regulations lead to a high rate of non-compliance on the part of the blood banks, compromising the quality and safety of transfusion services.
8. Ineffectiveness in enforcement of current legislature provides a breeding ground for flourishing Blood Mafia Market in India
India has made significant progress towards management of the blood infrastructure through eRakt Kosh under the National Health Mission (NHM) in April 2016. It is an integrated blood bank management information system which is a web-based mechanism that collects all blood banks of the state in one single network and adopts a total quality management approach. Despite this progress, the regulatory barriers to entry, unclear governing responsibilities between the pharmaceutical controller and NACO/NBTC and Fragmented distribution of blood banks at the macro level and at the micro level, requirements of a replacement donors pose significant challenges in making the system more efficient and responsive to the demand in the market. This gap is then filled by illegal commercial donors. India’s illegal blood market can be thought of as a consequence which arises from market failure.
India’s illegal blood industry is worth Rs 300 crore and growing every day. Nearly a third of blood collected by banks comes from paid (Commercial/professional) donors.
The common ways in which an illegal blood market operates are the following:
Commercial Blood Donors: Professional or commercial donors that donate blood in exchange of money. They often linger outside hospitals waiting for patients and their families who are looking for blood or a replacement donor.
Nexus of blood traders: These are organised groups of people that form a network of voluntary or involuntary blood donors.
Blood Farms: These are rare instances when an organised group uses involuntary donors by trafficking vulnerable people and trapping them in a vicious circle - getting them to donate blood under false pretences and taking out more blood than what is medically permitted and quite often thus rendering them very weak so that they are unable to escape. For example, the Gorakhpur blood farm which was raided by the police.
It is the lack of economic resources and opportunities that motivates people to sell blood for money. People who require blood for treatments often do not care for the origin of such a commodity. Doctors also act as referrals for these organisations or professional donors as they feel that it is the lesser of two evils.
8.1. Repercussions from Illegal Blood Market
High Risk of Diseases: While the blood supply increases on a short-term basis, there is a significant deterioration in the quality of blood with a high risk of infections like HIV, Hepatitis C.
Adulterated Blood Supply: People receive a low-quality blood, sometimes even diluted with water.
Plightful condition of Professional Donors: Vulnerable groups like informal immigrants are taken advantage of under the pretext of earning extra money.
Aggravation of Regional Disparity: People in the rural areas are more vulnerable to the illegal blood market as they have limited access to blood banks thereby, making them reliant on lower quality blood from illegal sources.
In October 2015 a major modification to the National Blood Policy now allows inter-bank transfer of blood, which is a big step towards bridging the supply-demand gap. In addition to that, the government now allows the hospital to hold blood donation camps, thereby reducing their dependence on replacement donors.
9. Paving the way forward to a blood-sufficient India
The paper has explored several issues that are leading to a fractured blood management system. The legal, distributional and supply chain inefficiencies are compromising the infrastructure, thereby giving space for an illegal market to thrive. The paper explores several possible recommendations to overcome some of these problems
9.1. Increasing Blood Supply by creating a pleasant donation experience for blood donors & minimising blood discard
Recommendations to increase both first-time donations and repeat donations to increase the quantity of blood donated voluntarily, are as follows:
Training medical staff to increase professionalism of behaviour: The staff must be trained, courteous and proficient at interpersonal communication. They should attend to the donors with a pleasant attitude, listen to their worries, complaints and suggestions and dispel their myths and fears, fostering better donor retention.
Improving the user experience donating blood, in blood donation centres: The blood donation centres must carry out user journey mapping and assessment to determine the areas of improvement of the blood donation experience. This will highlight the exact causes of donation deterrents like long waiting time, unpleasant atmosphere and perhaps even the poor behaviour of the medical staff.
Promoting mainstream awareness of blood donation: it’s How, When, Where Why - Such mainstream awareness must be based on 2 rationales:
Drawing attention to the scarcity of existing blood
Dispelling myths about the blood donation process
The promotion must be of high memorability with a strong call-to-action so that the crucial nature of blood donation lingers in mainstream consciousness and creates an ever-increasing number of donations. The advent of social media, and the widespread presence of almost every demographic on it, makes this promotion potentially low-cost.
This promotion of blood donation could emphasise on the following motivators for blood donation, that have been identified by the research papers:
Doing something conducive for the community out of altruism
Being encouraged by friends and family to donate blood
Donating blood as a peaceful protest for a cause
Satisfying the curiosity of how blood donation works and feels
Better management of blood components post-donation will ensure lowered blood wastage. Moreover, continued medical education and more hands-on training for technical staff is necessary. The training needs to be given on maintaining self-audits, tracking quality indicators of processing, and preparation of the blood components. This will minimise the discard rate of collected blood hence saving this scarce resource.
9.2. Regulation and Governance to be revisited
The Drugs and Cosmetics Act (DCA) and National Blood Transfusion Services Act (NBTSA) should be examined regularly to keep up with developing circumstances and new advancements in research. The transparency between the responsibilities of the drug controller of India and NACO/NBTC should be increased with NACO/NBTC assuming a role beyond advisory capacity.
The dual licensing system between the state and the central government could be relaxed, leading to reduced barriers to entry and the licensing process should be streamlined so that permits can be granted or renewed in as little as three months.
Many rural clinicians seek to address the issue of blood volume shortage through unbanked directed blood transfusion (UDBT) in which donors undergo rapid testing for transfusion-transmitted infections (TTIs). In India, UDBT has been illegal despite promises by the Drug Technical Advisory Board to legalise the procedure. Moreover, the 2015 National Health Policy acknowledged that UDBT is the only feasible and safe option in some contexts. With appropriate regulation and guidelines for safety and reporting, UDBT may be an appropriate way to help address the unmet need for blood in the rural setting.
9.3. Ensuring equitable, accessible and unrestricted Blood distribution network
It is imperative to extend the services of blood banks and storage centres to smaller towns and rural areas by both increasing functionality of blood storage centres and decreasing the current blood bank statutory requirements. To achieve this end, blood storage centres should be made fully functional, without the handicap of a replacement unit requirement.
Walking Blood Banks: Rural practitioners can utilise unbanked blood transfusions from a voluntary pool of pre-screened donors. This system would provide safe blood - as evidenced by international experience and limited projected increase in transfusion-transmissible infection in India - at a fraction of the financial cost imposed by the current system.
9.4. Use of technology like Big data and Blockchain to find smarter solutions
With the advancement of technology within the country and the increase of focus on medical technology, the nation does not lack capacity at those skills, most of the issues are management issues that require a lot of data that would help define the problem statement and opening avenues for data-driven decision making. This philosophy is already placed under the National Blood Policy 2007. This can be an opening of a commercial avenue especially in the health sector which have been traditionally a less focus in Big Data and Disruptive technology. This also connects with the past recommendations as an enabling mechanism.
Estonia, a country that is heavily involved in the using and applying new technologies presents a case that can be studied especially using Big Data and using a nation-wide KSI Blockchain cluster to aid the government and health sector.

Figure 9: KSI in blockchain
Using disruptive technologies like Blockchain, certain solutions like [19] (developed by Indian researchers specifically for the Indian system) can also be used for trailing information from donation to consumption, while also providing rich data to be generated and categorised in a fast manner for analysis. This also brings a higher transparency in the system and improves trust.
The key issue of Blood donor retention and gaining more donors for blood can be modelled as the same issue for gaining more customers and retaining most of them. This would cover a wide area in donation, starting from getting the donors to the donation centre (understanding the distance requirement and thus establishing a best location from a pool for blood centre) to understanding the colour of walls and how it affects retention and getting more donors, essentially forecasting the blood donors. These are just some examples and one can create a better place for data analytics in the healthcare sector which has not received much attention. Traditional tools like behavioural science and social sciences can also be combined to provide cross-functional solutions to the currently existing problems.

Figure 10
There has been much research into improving the blood safety process and some researchers have suggested data mining processes to do so that appears to be promising. It can also be used for reducing the discard.
A good mathematical model was recently developed by a professor in IIT Delhi which aims to curb the surplus and shortage across India by analysing the supply chain. It works in three fields: forecast the demand of blood units at the blood bank; determine the optimal allocation of units from blood banks with surplus to a blood bank with shortage; select the optimal route for the delivery of the allocations. This is an amazing solution to curb the distribution disparity.
10. Conclusion
Thus, through this paper, we have attempted to holistically understand the Indian blood industry by identifying current problems such as insufficient donors, poor retention rate, fragmented & inefficient distribution, ambiguous legal architecture & ineffective enforcement which provide a breeding ground for an illegal blood market to thrive in our country. To address these challenging issues, enhance the availability of BTS & ensure equitable blood distribution in our country, we have provided a set of recommendations which include making amendments to our legal infrastructure, improving data governance, using technologies like Big Data & Blockchain & finding smarter ways to increase blood donation & retention rate. We believe India can bridge the demand and supply gap for blood rapidly if these recommendations are put into action & its implementation is carried out smoothly.
Meet The Thought Leaders

Shatakshi Sharma has been a management consultant with BCG and is Co- Founder of Global Governance Initiative with national facilitation of award- Economic Times The Most Promising Women Leader Award, 2021 and Linkedin Top Voice, 2021.
Prior to graduate school at ISB, she was Strategic Advisor with the Government of India where she drove good governance initiatives. She was also felicitated with a National Young Achiever Award for Nation Building. She is a part time blogger on her famous series-MBA in 2 minutes.

Naman Shrivastava is the Co-Founder of Global Governance Initiative. He has previously worked as a Strategy Consultant in the Government of India and is working at the United Nations - Office of Internal Oversight Services. Naman is also a recipient of the prestigious Harry Ratliffe Memorial Prize - awarded by the Fletcher Alumni of Color Executive Board. He has been part of speaking engagements at International forums such as the World Economic Forum, UN South-South Cooperation etc. His experience has been at the intersection of Management Consulting, Political Consulting, and Social entrepreneurship.

Aashi Agarwal is a mentor at GGI and is currently working as a consultant at Kearney. She exhibits keen interest in the social sector and has gained vivid experiences being a part of Teach for India, Katalyst and BloodConnect Foundation. Aashi pursued her B.Tech from IIT Delhi and was conferred with the prestigious Director’s Gold Medal for her excellent all-rounder performance and leadership skills. Outside of work, you can find her writing poetry Slam, learning French or exploring new places, food, lifestyle and culture.
Meet The Authors (GGI Fellows)

Kavya Sangam is a final-year Bachelor of Economics student at SP Jain School of Global Management. She has worked internationally across numerous business sectors: hospitality, pro-bono consultancy, virtual corporate volunteering and journalism. She is also passionate about the welfare of the environment and society. In line with this, she has co-founded the website The Better You (www.thebetteryouu.com) where she writes about incorporating sustainability and self-development into our day-to-day lives.

Shreya Agarwal is an international development enthusiast, currently employed at Adam Smith International (ASI) in a hybrid business development and project management role. As a part of UNGC’s Young Sustainable Development Goals (SDG) Innovator Programme (YSIP), she and her team are implementing a Preferential Procurement Framework prioritising businesses owned by minority communities, women and social entrepreneurs across ASI’s global procurement process and building capacity of the suppliers to increase their competitiveness in the market. She has an M.Sc. in International Management degree from ESADE Business School and is keen on building her career in Impact Consulting.

Lakshya is a 3rd year student at BITS Pilani, Pilani Campus who would be graduating in 2023 with a B.E. Computer Science. He is currently a researcher in Computer Vision Team of Sally Robotics, an autonomous vehicle student-run club. Self-describing as an avid learner, jack of all trade and obsessed with efficiency, he is a person who wants to create a better world for the human race that would present an equality of opportunity for all and would help people realize their responsibilities.

Abhijit Choksi is an Aspirational District Fellow, working as a Niti Aayog consultant to the district administration/collector in Rajgarh, Madhya Pradesh. He’s also pursuing a public policy course from the Takshashila Institution currently. After finishing his BTech in Information Technology from NMIMS, Mumbai, he worked as a Teach For India fellow in Mumbai. He then prepared for the arduous civil services exam for 3 years. He is extremely passionate about working in the development sector & creating a grassroots level impact. He loves playing sports like tennis, cricket and basketball in his leisure.
Bibliography:
[1] National Estimation of Blood Requirement in India. National Aids Control Organization (NACO), 2018, www.naco.gov.in/sites/default/files/Final%20Estimation%20Report%20of%20Blood%20Requirement%20in%20India%20(1).pdf
[2] World Health Organisation. “Blood safety and availability 2020”, https://www.who.int/en/news-room/fact-sheets/detail/blood-safety-and-availability
[3] Global status report on blood safety and availability 2016. Geneva: World Health Organisation; 2017. Licence: CC BY-NC-SA 3.0 IGO.
[4] Saha, Shantanu, and Bibhas Chandra. "Influence of Age and Education on Blood Donation: A Qualitative Research." Studies on Ethno-Medicine 10.4 (2016): 425-435.
[5] Saha, S., and B. Chandra. "Study on identification of the factors impacting blood donation in Jharkhand, India." Indian J Fundam Appl Life Sci 5 (2015): 1-4.
[6] Shrivastava, Manisha et al. “Blood donor selection and deferral pattern as an important tool for blood safety in a tertiary care hospital.” Asian journal of transfusion science vol. 10,2 (2016): 122-6. doi:10.4103/0973-6247.187938
[7] zarin s bharucha. "Voluntary Blood Donation by 2020, Still a Gap to Be Bridged." @businessline, 1 Feb. 2020, www.thehindubusinessline.com/specials/pulse/voluntary-blood-donation-by-2020-still-a-gap-to-be-bridged/article30705752.ece. Accessed 10 Dec. 2021.
[8]Jenny, Hillary E., et al. "Access to safe blood in low-income and middle-income countries: lessons from India." BMJ Global Health 2.2 (2017): bmjgh-2016.
[9] Sood, Rachita, et al. "Walking blood banks: an immediate solution to rural India's blood drought." Indian journal of medical ethics 3.2 (2017): 134-137.
[10]Global status report on blood safety and availability 2016. Geneva: World Health Organisation; 2017. Licence: CC BY-NC-SA 3.0 IGO.
[11] Kanani, Ashishkumar Nathabhai, et al. "Analysis on discard of blood and its products with suggested possible strategies to reduce its occurrence in a blood bank of tertiary care hospital in Western India." Global Journal of Transfusion Medicine 2.2 (2017): 130.
[12] Jariwala, Keyuri, et al. "Reasons for discarding of whole blood/red cell units in a Regional Blood Transfusion Centre in Western India." Indian Journal of Hematology and Blood Transfusion 34.3 (2018): 501-505.
[13] Patil, Parikshit, Arvind Bhake, and Kishor Hiwale. "Analysis of discard of whole blood and its components with suggested possible strategies to reduce it." Int J Res Med Sci 4.2 (2016): 477.
[14] Das, Tina. "On World Blood Donor Day, a Look at India's Blood Crisis That's Compounded by Covid." ThePrint, 14 June 2020
[15] India. The Drugs and Cosmetics Act, 1940. Act, no. 194023, 10 Apr. 1940, www.cdsco.gov.in/opencms/export/sites/CDSCO_WEB/Pdf-documents/acts_rules/2016DrugsandCosmeticsAct1940Rules1945.pdf. Accessed 4 Dec. 2021.
[16] Sehgal, Diganth Raj. "All about blood donation in India - iPleaders." iPleaders, 16 Sep. 2021, blog.ipleaders.in/blood-donation-india. Accessed 4 Dec. 2021.
[17] "World Blood Donor Day 2017: Shocking Facts On India’s Illegal Blood Donation Industry." Moneycontrol, 14 June 2017, www.moneycontrol.com/news/trends/health-trends/world-blood-donor-day-2017-shocking-facts-on-indias-illegal-blood-industry-2304179.html. Accessed 4 Dec. 2021.
[18]Luhar, R. K., and R. J. Shah. "Discard rate in blood transfusion service–A critical tool to support blood inventory management." (2020).
[19] Lakshminarayanan, Sivakamy, P. N. Kumar, and N. M. Dhanya. "Implementation of Blockchain-Based Blood Donation Framework." International Conference on Computational Intelligence in Data Science. Springer, Cham, 2020.
[20] Kauten, Christian, et al. "Predicting Blood Donors Using Machine Learning Techniques." Information Systems Frontiers (2021): 1-16.
[21] Marade, Chinmay, et al. "Forecasting Blood Donor Response Using Predictive Modelling Approach." (2019).
[22] Ferguson, Eamonn, et al. "Improving blood donor recruitment and retention: integrating theoretical advances from social and behavioural science research agendas." Transfusion 47.11 (2007): 1999-2010.
[23] Erraguntla, Madhav, et al. "Data Mining to Improve Safety of Blood Donation Process." 2014 47th Hawaii International Conference on System Sciences. IEEE, 2014.
[24] Rad, Jaber, et al. "An AI-Driven Predictive Modelling Framework to Analyse and Visualise Blood Product Transactional Data for Reducing Blood Products’ Discards." International Conference on Artificial Intelligence in Medicine. Springer, Cham, 2020.
[25] Guan, Leying, et al. ``Big data modelling to predict platelet usage and minimise wastage in a tertiary care system." Proceedings of the National Academy of Sciences 114.43 (2017): 11368-11373.
[26] Dharmaraja, S., Srijan Narang, and Vidyottama Jain. "A mathematical model for supply chain management of blood banks in India." Opsearch 57.2 (2020): 541-552.
[27]Aparna, Meduri. "Article 21 of Indian Constitution-Mandate for Life Saving." Available at SSRN 906704 (2006).
[28] Dhot, P. S. "Amendments to Indian drugs and cosmetics act and rules pertaining to blood banks in armed forces." Medical journal, Armed Forces India 61.3 (2005): 264
[28] Carney, Scott. Red Market. Hachette UK, 2012.
[29] World Health Organisation. Blood donor selection: guidelines on assessing donor suitability for blood donation. World Health Organisation, 2012.
[30] Das, Kunal, et al. "Indian blood donor selection guidelines: Review in the context of the ongoing COVID-19 pandemic." Transfusion Clinique et Biologique (2021).
[31] Baş, Seda, et al. "Management of blood donation system: literature review and research perspectives." Health care systems engineering for scientists and practitioners (2016): 121-132.




Comments